Nanotechnology affects every aspect of the health sciences. There are now such subject areas as Nanobiotechnology and DNA Nanotechnology. Engineered vaccines contain proteins with nanoscale dimensions. Here we'll focus on the broader classification of nanomedicine which includes examples of nanopharmaceutials. Nanopharmaceuticals and nanomedicine are vast areas of expertise which are developing at an impressive rate. Here are some of the major advances which nanotechnology has brought to these fields.
Nano-particles and Nano-encapsulation
Metal nanoparticles, carbon nanotubes, polymers can be used in different ways in medicine especially when combined with antigen-specific coatings or functional groups on their surfaces. Their size, physical properties and chemical composition determine their usefulness. The small size of these structures lends itself to their use and ease of circulation but they mustn’t get lodged in capillaries and other microanatomies.
Nanoparticles for Medical Imaging
Nanoparticles have been used as contrast and image enhancing agents for x-ray and computed tomography (imaging via any kind of penetrating wave) imaging (CT). Conventional methods of imaging use iodinated benzoic acid derivatives but these have risk factors and side effects associated with intravenous iodine injection. These derivatives are of low molecular weight so clear from the body rapidly and are difficult to direct to disease sites. Iodinated molecules have been encapsulated to overcome these problems but stability and concentration of agent delivered to imaged site is low.
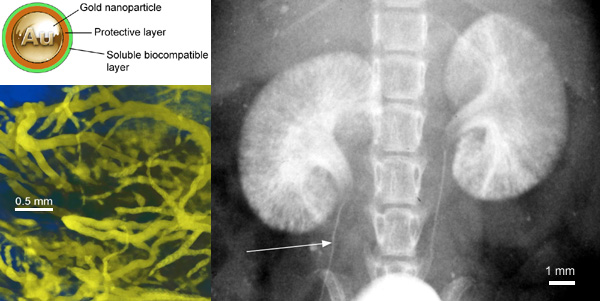
In order to enhance an X-ray image an agent must deliver detectable numbers of heavy atoms into the imaged tissue without toxic effects. Suitable nanoparticles are those made of elemental heavy metals such as gold as these have high densities and are still biologically inert and stable. To overcome the cost issue associated with gold researchers at General Electric developed nanoparticles made of heavy metal compounds encapsulated in gold shells. By adding thiol groups gold nanoparticles can be coated with selectively binding antigens, antibodies or target compounds for receptor on the surfaces of cells. By targeting receptors unique to certain types of cancer cells, gold nanoparticles can be made to enhance an x-ray image by increasing the ability to detect the the cancer cells by many orders of magnitude.
Nanoparticles for Medical Imaging
Nanoparticles have been used as contrast and image enhancing agents for x-ray and computed tomography (imaging via any kind of penetrating wave) imaging (CT). Conventional methods of imaging use iodinated benzoic acid derivatives but these have risk factors and side effects associated with intravenous iodine injection. These derivatives are of low molecular weight so clear from the body rapidly and are difficult to direct to disease sites. Iodinated molecules have been encapsulated to overcome these problems but stability and concentration of agent delivered to imaged site is low.
In order to enhance an X-ray image an agent must deliver detectable numbers of heavy atoms into the imaged tissue without toxic effects. Suitable nanoparticles are those made of elemental heavy metals such as gold as these have high densities and are still biologically inert and stable. To overcome the cost issue associated with gold researchers at General Electric developed nanoparticles made of heavy metal compounds encapsulated in gold shells. By adding thiol groups gold nanoparticles can be coated with selectively binding antigens, antibodies or target compounds for receptor on the surfaces of cells. By targeting receptors unique to certain types of cancer cells, gold nanoparticles can be made to enhance an x-ray image by increasing the ability to detect the the cancer cells by many orders of magnitude.
In the journal Angewandte Chemie ("Phosphorescent Nanoscale Coordination Polymers as Contrast Agents for Optical Imaging"), a team led by Wenbin Lin at the University of North Carolina, Chapel Hill, USA, in March 2011 introduced a novel contrast agent that marks tumor cells in vitro. The dye is a phosphorescent ruthenium complex incorporated into nanoparticles of a metal–organic coordination polymer, which allows an extraordinarily high level of dye loading.
Fluorescent dyes accumulate in varying amounts in different types of tissue. Such contrast agents make it possible to use optical imaging to
differentiate between healthy and tumorous tissue. However, this method is limited by the fact that very high concentrations of dye are needed to produce
sufficiently strong fluorescence. Organic dye molecules packed at high concentrations into nanocapsules tend to quench each other's fluorescence.
Materials that fluoresce more strongly, such as quantum dots, are often not biocompatible.
Fluorescent dyes accumulate in varying amounts in different types of tissue. Such contrast agents make it possible to use optical imaging to
differentiate between healthy and tumorous tissue. However, this method is limited by the fact that very high concentrations of dye are needed to produce
sufficiently strong fluorescence. Organic dye molecules packed at high concentrations into nanocapsules tend to quench each other's fluorescence.
Materials that fluoresce more strongly, such as quantum dots, are often not biocompatible.
Nanoparticles for Targeting Cancer cells

Nanoparticles that detect cancer cells in blood stream
This is a rapidly advancing area of research. Cancer cells are released into the blood stream in large numbers by microscopic tumours too small to be detected by imaging modalities. If these could be detected and concentrated from a blood test it would provide a means of early detection of cancer before tumours were big enough to be detected by imaging. This would lead to a much better prognosis for cancer patients. To do this ferromagnetic micro- and nanoparticles are functionalized with antibodies, allowing cancer cells to be separated out of tissue samples such as concentrated blood for diagnostic analysis. [39]
Nanomagnetic particles can be used also for magnetic controlled drug targeting. It works by binding these particles to anti-cancer drugs which allows them to accumulate in one area. Eg. At a tumour by means of a magnetic field. The drug then desorbs from the ferrofluid and attacks the tumour. Magnetic particle separation can also be used to separate cancer cells from bone marrow and other tissues, and for the isolation, identification and genetic analysis of specific DNA sequences. [42]
Nanomagnetic particles can be used also for magnetic controlled drug targeting. It works by binding these particles to anti-cancer drugs which allows them to accumulate in one area. Eg. At a tumour by means of a magnetic field. The drug then desorbs from the ferrofluid and attacks the tumour. Magnetic particle separation can also be used to separate cancer cells from bone marrow and other tissues, and for the isolation, identification and genetic analysis of specific DNA sequences. [42]
Nano-Encapsulation for Drug Delivery to Tumours
|
Nanoparticles can be filled with absorbed or encapsulated drugs and targeted onto cancer cells or disease agent. The aim is to deliver nanoparticles with concentrated anti-cancer drug straight to the tumour site without affecting healthy cells. Drug laden nanoparticles can be injected into tumours with procedures that are minimally invasive. Their effect can be enhanced by using drugs that are further activated by radiation. Some of these drugs may have problems getting to the tumour site due to physiochemical properties, including high toxicity, and so it helps for them to be embedded directly in to the tumour. When the encapsulated drug is embedded in the tumour the polymer and nanoparticle shell are degraded for the controlled release of the highly toxic chemotherapeutic drug into the tumour, without affecting other tissues. The video on the right describes this process in simple terms with good animations which help explain the concept.
|
|
An example of an anti-cancer drug that can be enhanced by nanoparticle drug delivery is β-lapachone. This is a napthoquinine found in the bark of a South American tree which induces cytotoxic effects in malignant human cell types such as colon, lung, prostate, breast, pancreatic, ovarian and bone cancers as well as some blood cancers and cancer of the retina (retinoblastoma). They found that β-lapachone interacts with an enzyme which is present in high levels in some types of solid cancer tumours. In tumours the drug is metabolized and the metabolite kills the tumour. Normal cells are not affected as they don’t contain the enzyme. But the problem is that when this drug is injected into the tumour it is carried away rapidly in blood circulation. Dr. Boothman and his group in the University of Texas are developing a variety of polymer implants that can be placed in the tumour to slowly release the anticancer drug in an effective manner. The implants included nanoscale polymer drugs moulded from nanocells derived from a number of natural nanomaterials: [41]
Nanoencapsulation for Penetration of Blood Brain Barrier
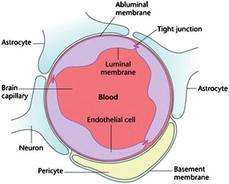
The Blood Brain Barrier
In the central nervous system epithelial cells lining the walls of blood vessels overlap in tight junctions, unlike those in the rest of the body. This closes off easy transport of large molecules (about 500DA molecular weight) between blood and brain. This helps protect the sensitive and vital central nervous system from disturbance by chemicals and pathogens (e.g. viruses).
The barrier is lipophillic. To get past molecules must be small and lipophillic. Many of the drugs designed to treat diseases of the brain such as Alzheimer’s disease, Huntington’s disease, stroke and brain cancer depend on carrier-mediated transport and other such mechanisms to cross the blood brain barrier.
Nanotech offers a possible alternative for transport through the blood brain barrier that is more generally applicable to a wide range of drugs. Drugs can be encapsulated in biodegradable polymers to make artificial liposomes. The coatings contain active sites to which antibodies can be attached. The antibodies are recognised by the brain capillary brain receptors, which mediate their passage through the blood brain barrier. Once inside the liposomes release the drug. [42]
The radio labelled Cu2+ or Fe3+ metal chelator clioquinol, which has a high affinity for plaque which is a factor in neurodegenerative disease, has been encapsulated in liposomes capable of crossing the blood brain barrier.
The fact that some nanoparticles cross the blood brain barrier could be as much of a curse as it is a blessing. The blood brain barrier protects the brain from toxic chemicals that could damage it and the fact that nanomaterials can cross this barrier is a worry for some doctors.
The barrier is lipophillic. To get past molecules must be small and lipophillic. Many of the drugs designed to treat diseases of the brain such as Alzheimer’s disease, Huntington’s disease, stroke and brain cancer depend on carrier-mediated transport and other such mechanisms to cross the blood brain barrier.
Nanotech offers a possible alternative for transport through the blood brain barrier that is more generally applicable to a wide range of drugs. Drugs can be encapsulated in biodegradable polymers to make artificial liposomes. The coatings contain active sites to which antibodies can be attached. The antibodies are recognised by the brain capillary brain receptors, which mediate their passage through the blood brain barrier. Once inside the liposomes release the drug. [42]
The radio labelled Cu2+ or Fe3+ metal chelator clioquinol, which has a high affinity for plaque which is a factor in neurodegenerative disease, has been encapsulated in liposomes capable of crossing the blood brain barrier.
The fact that some nanoparticles cross the blood brain barrier could be as much of a curse as it is a blessing. The blood brain barrier protects the brain from toxic chemicals that could damage it and the fact that nanomaterials can cross this barrier is a worry for some doctors.
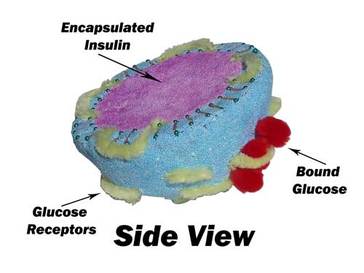
Nanoparticles and Nanoencapsulation for Insulin
The main cause of Type I (insulin dependent) diabetes mellitus is degradation of insulin- producing cells in the Islets of Langerhans. Insulin must be injected to treat this disease because it is a peptide and will be broken down by digestive enzymes. There are risks of improper dosage and rates of release related to the administration route. Insulin needs to be released in controlled amounts.[42]
Nanoencapsulation for the Protection of Implants from the Immune System
Most work on transplanting encapsulated cells has been in the area of insulin- producing pancreatic beta cells. After years of having experiments that result in the implants being smothered by plaques and invaded by the immune system of the host, promising results are beginning to appear using new nanoengineered encapsulation materials and techniques. Encapsulation of pancreatic islets allows for transplantation in the absence of immune-suppression.[43]
Most work on transplanting encapsulated cells has been in the area of insulin- producing pancreatic beta cells. After years of having experiments that result in the implants being smothered by plaques and invaded by the immune system of the host, promising results are beginning to appear using new nanoengineered encapsulation materials and techniques. Encapsulation of pancreatic islets allows for transplantation in the absence of immune-suppression.[43]
Guiding and Stimulating Tissue Function and Growth
Tissue scaffolding or tissue engineering is an emerging technique in surgery and wound healing which is being given new options by the development of new nanomaterials and nanostructures. There are nanotechnologies aimed at bridging the nerve generation gap which may one day be applied to restore mobility to patients with spinal nerve column damage. Nanotechnology can help reproduce or repair damaged tissue. “Tissue engineering” makes use of artificially stimulated cell proliferation by using suitable nanomaterial-based scaffolds and growth factors. For example, bones can be regrown on carbon nanotube scaffolds. Tissue engineering
might replace today's conventional treatments like organ transplants or artificial implants. Advanced forms of tissue engineering may lead to life extension.The area of nanoguides for neural growth and repair is a very diverse and complicated area of research in which a lot of work is being done.[42]
might replace today's conventional treatments like organ transplants or artificial implants. Advanced forms of tissue engineering may lead to life extension.The area of nanoguides for neural growth and repair is a very diverse and complicated area of research in which a lot of work is being done.[42]
Neuronal Stimulation and MonitoringNanotechnology advances devices such as cardiac pacemakers, cardiac defibrillators, cochlear implants, bone growth stimulators and neural stimulators with improved battery technologies, biocompatible materials, and surface treatments for enclosures and leads electrode miniaturizations and efficiency improvements, and smaller sized integrated circuits for control and power, while speed and processing capabilities increase. [42]
Leg, Knee, Foot and Hand Prostheses This is a very active and exciting area for application of new nanotechnology. Miniature electronic motors or pneumatic muscles have yet to be replaced by nanoengineered artificial muscles in an integrated design for an artificial hand. The realm of neuroplastics is one being implicated by nanotechnology on many different levels. This field again is very broad and complex. [42]
|
Neuroprosthetics
Neural interfaces to nano- and micro- electronic devices open new opportunities to design more powerful neurostimulators for prosthetics.
Nanotechnology will have a great impact on medicine with assemblies of cooperating interconnected networks of computing, communicating and sensing nanoprocessors driving assemblies of modular interworking nanoactivators to make up a micro- or macro- device like a subtle but powerful motor neuroprostheses. For example glasses and external hearing aids are prostheses, but a sensory neuroprotheses is an active device that delivers electrical stimulus to the nervous system, such as cochlear (ear) implants or artificial retina. Applications of nanotechnology may come up with convenient, low-cost nanoengineered smart acoustical materials that could filter out damaging frequencies and noise levels for ear prostheses. [42] Visual Neuroprostheses
|
Diagnostics; Lab-on-a-Chip
|
These little devices could quite possibly be the most widely useful piece of equipment which nanotechnology has allowed scientists to create. At the moment in doctors surgerys everywhere patients are giving blood samples and are then sent away to wait for results for a few days. Labs-on-chips would eradicate this waiting period as they allow a tiny drop of blood to be tested immediately and results to be given there and then in the doctors surgery. Some have already been created such as the one for diagnosing HIV. The advancement in nanotechnology has made it possible for you to have an entire medical lab reduced down to the size of a high-powered chip. Researchers are working hard towards creating a nano sized lab that performs a variety of tasks. These tasks signify conducting multiple diagnostic tests, which would take an entire team of doctors, at least, a week to provide results. The reason they have not been widely available yet is because of the cost issues. But in the long term it would seem costs would balance out with the money saved on not needing as many full-scale labs and analysts.
|
|
Examples of advances in nano chips: Magnetic nanoparticles, bound to a suitable antibody, are used to label specific molecules, structures or microorganisms. Gold nanoparticles tagged with short segments of DNA can be used for detection of genetic sequence in a sample. Multicolor optical coding for biological assays has been achieved by embedding different-sized quantum dots into polymeric microbeads. Nanopore technology for analysis of nucleic acids converts strings of nucleotides directly into electronic signatures. [8]
Diagnosis of HIV on a Chip
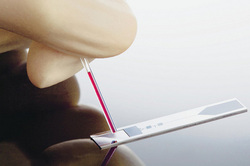
Lab on a Chip for testing of HIV
The Guardian, in their article, “The incredible shrinking laboratory or lab-on-a-chip”, states that Professor Tom Duke of the London Centre of Nanotechnology is working on a “lab-on-a-chip” to test HIV. In this chip, nanometer-sized pillars separate a drop of blood in such a way that the larger elements such as blood cells and proteins are trapped. The virus particles then pass through this trap where the come across a series of levers that are coated with antibodies. These antibodies then tend to bend when hit. The more they bend indicates the amount of virus present. This is just one application that the lab-on-a-chip possess. There are many other features that are also present.
The LOC will be of big benefit to developing countries where full-scale laboratories are not accessible.
The LOC will be of big benefit to developing countries where full-scale laboratories are not accessible.
Treatment of Tuberculosis
|
The WHO estimates that approximately one-third of the global community is infected with M. tuberculosis. In 2006, an estimated 9.2 million incident cases and approximately 1.7 million deaths due to TB occurred worldwide making it the worlds leading causes of mortality. The safety and uptake of the nanoparticles is being tested in TB-infected mice and the effectiveness of the nanodrug is being compared to conventional therapy to see whether a weekly nano dose is as effective as the standard daily treatment regime. Human trials for the antibiotic, called Rifanano, are scheduled for this year. |
Diagnostics: The Central Scientific Instruments Organization of India designed a nanotechnology-based TB diagnostic kit, which is currently in the clinical trials phase. This kit does not require skilled technicians for use and offers portability, efficiency, user-friendliness and availability for less than US$1. The research is also ongoing for an optical biosensor for rapid TB detection in the Medical Sciences division of the U.S. Department of Energy. Another group at RMIT University, in Australia, is conducting research into the application of novel tethered nanoparticles as low-cost, colour based assays for TB diagnosis.
Treatment: The micro-encapsulation of pharmaceutical substances in biodegradable polymers used in controlled drug delivery has seen
as an emerging technology. Carrier or delivery systems such as liposomes and microspheres have been developed for the sustained delivery of anti-TB drugs and
have found better chemotherapeutic efficacy when investigated in animal models (e.g. mice).
TB Vaccination, The aerosol vaccine- under development through collaboration between Harvard University and the international not-for-profit Medicine in Need
(MEND) - could provide a low-cost, needle-free TB treatment that is highly stable at room temperature. While most new TB vaccines continue to call for
needle injection, but this new vaccine could provide safer, more consistent protection by eliminating these injections and the need for refrigerated storage. [44]
Treatment: The micro-encapsulation of pharmaceutical substances in biodegradable polymers used in controlled drug delivery has seen
as an emerging technology. Carrier or delivery systems such as liposomes and microspheres have been developed for the sustained delivery of anti-TB drugs and
have found better chemotherapeutic efficacy when investigated in animal models (e.g. mice).
TB Vaccination, The aerosol vaccine- under development through collaboration between Harvard University and the international not-for-profit Medicine in Need
(MEND) - could provide a low-cost, needle-free TB treatment that is highly stable at room temperature. While most new TB vaccines continue to call for
needle injection, but this new vaccine could provide safer, more consistent protection by eliminating these injections and the need for refrigerated storage. [44]
New Biomaterial
A new biomaterial designed for repairing damaged human tissue doesn't wrinkle up when it is stretched. The invention from nanoengineers at the University of California, San Diego marks a significant breakthrough in tissue engineering because it more closely mimics the properties of native human tissue.
Shaochen Chen, professor in the Department of NanoEngineering at the UC San Diego Jacobs School of Engineering, hopes future tissue patches, which are used to repair damaged heart walls, blood vessels and skin, for example, will be more compatible with native human tissue than the patches available today. His findings were published in a recent issue of the journal Advanced Functional Materials.
The team includes postdoctoral researchers in multiple disciplines: David Fozdar with the University of Texas at Austin, Department of Mechanical Engineering; Li-Hsin Han with the Stanford University School of Medicine, Department of Orthopeadic Surgery; and Pranav Soman and Jim Woo Lee at the UCSD Jacobs School of Engineering Department of NanoEngineering. [45]
Shaochen Chen, professor in the Department of NanoEngineering at the UC San Diego Jacobs School of Engineering, hopes future tissue patches, which are used to repair damaged heart walls, blood vessels and skin, for example, will be more compatible with native human tissue than the patches available today. His findings were published in a recent issue of the journal Advanced Functional Materials.
The team includes postdoctoral researchers in multiple disciplines: David Fozdar with the University of Texas at Austin, Department of Mechanical Engineering; Li-Hsin Han with the Stanford University School of Medicine, Department of Orthopeadic Surgery; and Pranav Soman and Jim Woo Lee at the UCSD Jacobs School of Engineering Department of NanoEngineering. [45]
In the Surgery
It's an endless list of ways in which nanotechnology is advancing medicine. Other areas such as robotic surgery and implantable sensors for blood pressure have also seen improvements. It's going to majorly affect, like all industries, communication devices, data storage, information displays and other instruments within the hospital.